Treatments for Spinal Compression Fractures
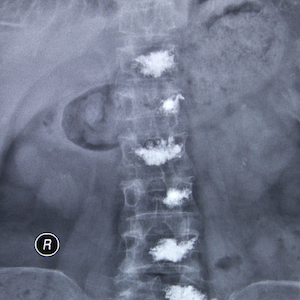
Osteoporosis, a disease that gradually weakens bones, causing them to become brittle, affects more than 28 million Americans. If not prevented or if left untreated, osteoporosis can progress painlessly until a bone breaks.
Along with hip and wrist fractures, severe osteoporosis can cause compression fractures in the spine. This occurs when the bony block, or vertebral body, in the spine collapses causing severe pain, deformity and loss of height.
Compression fractures occur in more than 700,000 patients per year in the United States, are more frequent than hip fractures, and often result in prolonged disability.
Until recently, doctors were limited in how they could treat osteoporosis-related spine fractures. Pain medications, bed rest, bracing or invasive spinal surgery were the only options available. Today there are two promising therapeutic and preventive treatments for compression fractures. They are called Vertebroplasty and Kyphoplasty.
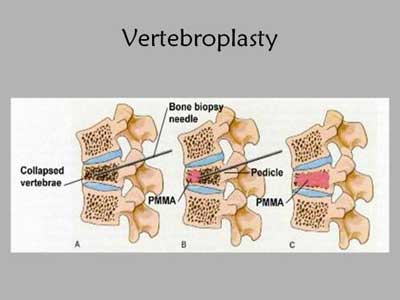
Vertebroplasty
Vertebroplasty was originally developed in France in 1986 and has been further refined and available in the United States since 1991. Vertebroplasty is a minimally invasive, non-surgical procedure that is designed to relieve the pain of compression fractures. Vertebroplasty literally means fixing the vertebral body. In addition to relieving pain, those vertebral bodies that are weakened but not yet fractured can be strengthened, thus preventing future problems.
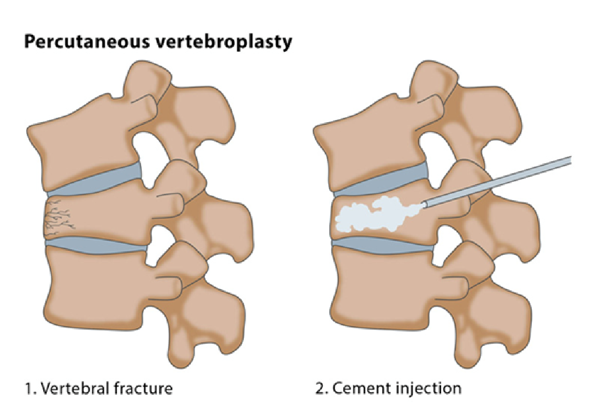
Percutaneous Vertebroplasty
Percutaneous Vertebroplasty is a procedure that helps relieve pain associated with compression fractures of the vertebral body, a thick block of bone located on the front of each spine vertebra. Osteoporosis, a disease that attacks bone and causes the spine to weaken and become brittle is one of the primary causes of compression fractures. The vertebral body becomes so thin that it can break from simple movements such as twisting, bending, and even coughing. The term "percutaneous" means injecting a fluid through a needle. "Plasty" means to mold or form. Thus, Vertebroplasty helps mold the vertebrae by injecting a fluid into the bone.
In this case, the doctor injects a bone cement mixture of polymethylmethacrylate (the same cement used in joint replacement surgery), barium or tantalum powder (makes the cement visible on X-ray), an antibiotic, and a solvent into the vertebral body. The cement will harden, strengthen and stabilize the vertebra, and prevent further collapse. In addition to relieving pain, those vertebrae that are weakened but not yet fractured, can be strengthened, thus preventing future problems. Most patients report pain relief within 24 to 72 hours and between 70% and 80% has sustained pain relief.
Procedure Overview:
Percutaneous Vertebroplasty is an outpatient procedure performed in the operating room or a special procedure room. When brought to the operating or special procedure room, you are connected to monitoring equipment (EKG monitor, blood pressure cuff, and a blood-oxygen monitoring device), and positioned on your stomach. The doctor or nurse will start an intravenous line and give some medicine to help you relax. Your back is cleansed with an antiseptic soap after which the doctor injects numbing medicine deep into your skin and tissue.
This will cause a burning sensation for a few seconds. A special bone needle is inserted into the vertebral body. With the assistance of a special X-ray machine called a fluoroscope, the doctor injects a radiopaque dye (contrast solution) to verify location of the needle. When the needle is in the correct position, the doctor will inject the cement mixture. During this time, you will not feel pain but you may feel some pressure. After the procedure, you will continue lying on your stomach for an hour or two. We ask that you remain at the Clinic until the doctor feels you are ready to leave.
Procedure Details:
Will you be asleep for the procedure? Normally, percutaneous vertebroplasty is performed with numbing medicine (local anesthesia) and other medication to keep you comfortable. Under special circumstances, the doctor may recommend that you go to sleep. How long will the procedure take? Percutaneous Vertebroplasty usually takes about 1-2 hours.
Before the procedure:
Do not eat or drink anything after midnight the day before the procedure. If you are on medications, you may take them with sips of water. If you are a diabetic, discuss your medication with the doctor. You may need to stop taking certain medications several days before the procedure. Please remind the doctor of all prescription and over-the-counter medications you take, including herbal and vitamin supplements. The doctor will tell you if and when you need to discontinue the medications. Tell the doctor if you develop a cold, fever, or flu symptoms before your scheduled appointment.
After the procedure:
The doctor may require that you wear a brace. If so, please follow the instructions. Keep the area clean and dry to help prevent skin infection. Do not do any heavy lifting for 3 months (i.e. nothing heavier than a carton of milk). After that, you can gradually increase your lifting to normal. Walking is encouraged and you can bend within the restrictions of your brace. You may experience some muscle discomfort where the needles were placed. This may be treated with a mild pain reliever such as Tylenol.
Do not drive for the remainder of the day. Please have an adult drive you home or accompany you in a taxi or other public transportation. Depending on how you feel, you may resume normal activities and return to work in one to three days.
Procedure Risks:
The risks are minimal and in fact, few complications have been reported. Potential complications include: infection at the injection site, bleeding, fractured rib, collapsed lung, worsened pain, and paralysis due to leakage of cement.